
If broached, peritoneal dialysis might be a better option
Many patients with end-stage kidney disease hear about in-center blood-cleansing, but not about the DIY approach at home.
It’s an unforgettable, life-changing moment when someone learns that their kidneys are functioning so badly that dialysis or a transplant will be necessary to survive.
“In some cases, the patient has lived with kidney disease for years and has known this day would come. With others, the disease has been mostly asymptomatic, so it is more of a shock. Either way, it is a difficult conversation. There is a sense of loss when organs fail,” said Dr. Raj Mehrotra, head of nephrology at the University of Washington School of Medicine.
That conversation is crucial to set the patient’s expectations about options for care and to empower that individual with information to decide which care makes the most sense, he said.
Given the gravity, it is disconcerting that one study of the patient population showed that 100% had been told about in-center hemodialysis, but only about 30% had been told of peritoneal dialysis, the stay-at-home, do-it-yourself option.
“The wheels of our healthcare system have long been greased to get patients into that hemodialysis chair,” Mehrotra said. “It is starting to change, but many people who might want to dialyze at home are not told they have that choice.”
With peritoneal dialysis, the abdominal lining (peritoneum) is used to filter waste products from blood. A cleansing fluid flows through a catheter into the abdomen, and the filtered waste fluid flows out and is discarded. This process requires several filtrations a day, which can be done at home on the patient’s schedule.
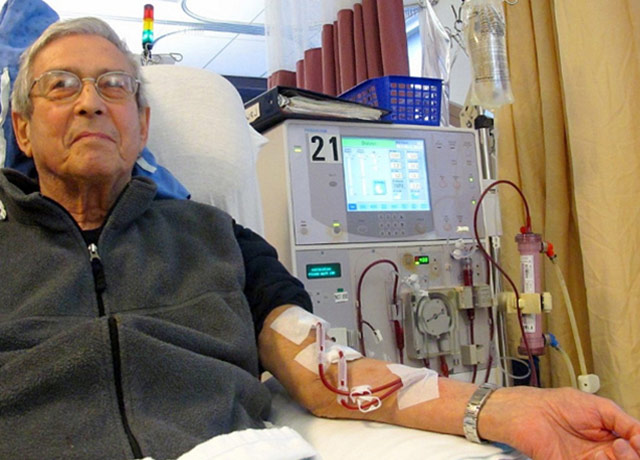
With hemodialysis, blood flows in and out of the body and is filtered by a machine. The thrice-weekly, three- to four-hour process conventionally happens with a clinician’s assistance during business hours at a dialysis center. A tiny portion (about 2%) of dialysis patients performs hemodialysis at home four to six days a week.
Of course, how a doctor presents these options can hugely influence a patient’s mindset. Some nephrologists filter their presentation through biases and paternalistic attitudes, Mehrotra said, about whether certain patients can manage the DIY regimen or should have the “privilege” of at-home dialysis.

"Some physicians don't trust the patient to make this decision, or they think patients' outcomes are better with in-center dialysis, though that is not borne out by data (1, 2).”
Missing from these scenarios is what Mehrotra calls “decision support.”
“The goal of the conversation is not to steer patients one way or the other, but to flesh out what's important to them. Some patients appreciate the socialization of an in-center unit (with other patients nearby) or simply may want a technician to manage the dialysis process,” he said. “Others don’t want to burden a family member with frequent drives to a center or they want more freedom to manage their own care.”
Research indicates that patients who are told about at-home dialysis are much more likely to opt for it. In the past decade, the number of at-home dialysis patients has roughly doubled — though it is still dwarfed by the 85-88% of dialysis patients who receive in-center care.
Now the U.S. government is trying to amplify that at-home growth trend.
The Centers for Medicare and Medicaid Services, armed with recent data showing that in-home dialysis is more affordable, last year began offering additional incentives to dialysis centers that show they are facilitating in-home care for patients.
To the extent that this experiment results in more patients ending up getting care that suits them, Mehrotra is supportive. “The growth of peritoneal dialysis in the United States tells me that our healthcare system is recognizing something important. But growing home dialysis in my mind is not an end in itself. It is the empowerment of patients to make that choice.”
Written by Brian Donohue - 206-543-7856, bdonohue@uw.edu
For details about UW Medicine, please see our About page.