
Tents, cars, bus stops are heart-failure treatment sites
By going into the community, building trust and stabilizing patients’ health, nurses reduce costly emergency visits and readmissions.Media Contact: Brian Donohue - 206-543-7856, bdonohue@uw.edu

On its face, a small mobile-care program in the Seattle metro area sounds mostly like a gesture of compassion from the county hospital: Clinicians make house calls to treat a few dozen citizens who struggle with life’s daily demands.
But look closer. Harborview Medical Center’s Community Heart Failure Program not only stabilizes patients’ cardiac health but also creates bottom-line value by reducing those patients’ admissions, lengths of stay and emergency-department visits.
“You’re trying to stay well, but you don't have transportation, or you’re in withdrawal or your mental illness is totally untreated. The idea that you'll get on a bus and show up promptly at 11:30 on a Tuesday is not realistic for many people,” said Jaimie Pechan, a UW Medicine heart-failure nurse practitioner and program cofounder.
“Most people want care,” she continued, “but the American healthcare system is not set up for them to be successful.”

Identifying an endless cycle
In 2016, Pechan and colleague Kate Smith, a heart failure registered nurse, recognized that some patients seemed caught in a cycle: They’d show up at Harborview’s Emergency Department in dire condition, get admitted, receive two weeks of resource-intensive care, get discharged — and never appear at a follow-up appointment. Then they’d be back in the ED.
“It just seemed like we needed a different way to reach these patients,” Smith said.
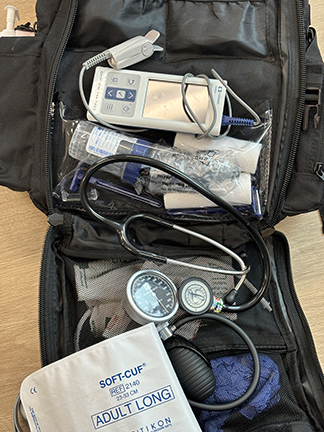
One day, with initiative borne of frustration, they put blood-draw supplies and a blood pressure cuff into a backpack and walked down into the neighborhood.
“It was natural and organic and kind of a no-brainer,” Smith said. “And today it’s this great program.”
In 2020, they got the administrative OK to spend a half-day a week treating a roster of 16 patients in supportive housing complexes and shelters downtown. Today, the mobile heart-failure program encompasses four days of their week and 60-some patients who live between Seattle’s north end and Auburn, 35 miles south.
‘I don’t think I would’ve made it this far.’

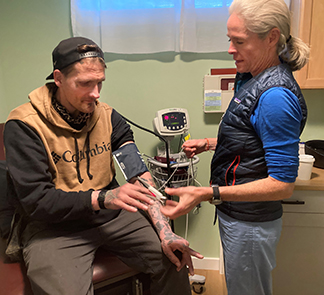
Appointments take place where the patient feels comfortable receiving care: apartments, tents, parking lots, bus stops, and back seats of cars. Today Pechan and Smith are on Seattle’s gritty Aurora Avenue North in the nondescript building that houses Aurora Commons, an organization that assists vulnerable people.
They are meeting with Michael Carpenter, their patient since early 2023.
Carpenter, 38, grew up in Everett, Wash., and moved to Seattle four years ago. He is trying to get his life in order after two decades of drug addiction. He appears healthy — strong enough to ride a motorcycle, anyway — but is quite sick, Smith confirmed. He has lived with heart failure for 15 years and attributes it to drug use and family genetics.
“There’s physical pain in my chest, like a cramp. I’m weak and fatigued and sometimes I can’t breathe. Sometimes it’s hard for me to get around. I don’t think I would’ve made it this far if they didn’t come to me,” he said, gesturing at his two nurses. “My life is way more stable now.”
Carpenter had his implanted defibrillator replaced in late 2022 but he continued to have dangerous heart rhythms and worsening heart failure. Past experiences with healthcare systems made him wary of seeking care, and his use of methamphetamine and fentanyl made attending appointments difficult. The heart team feared he would die without care, Pechan said.
She and Smith began seeing Carpenter weekly at Aurora Commons in January 2023. They focused on building trust and encouraged him to take his heart medications. After a serious hospital admission in April 2023, Carpenter decided to get sober. The heart team connected him with addiction specialists to aid his recovery. They coordinated his procedures and clinic visits, monitored his heart failure and adjusted his meds. He hasn’t been admitted to the hospital again.
Now he checks in with Smith and Pechan about every other week. He stopped using meth and fentanyl last year and gave up marijuana and cigarettes this year. The cup of coffee beside him is his last vice, he joked.
These efforts might someday make Carpenter eligible for a heart transplant, Pechan said. “At this point, a transplant is the only way he can get better.”
Hardships extend beyond taxing physical illness
Heart failure’s physical burdens are considerable. The heart’s weaker contraction means other vital organs and systems don’t get enough blood to function well. This brings crushing fatigue and shortness of breath. People swell with fluid that their bodies labor to flush out. They wheeze and cough and feel like they are drowning, Smith said.
These symptoms pose hardships for anyone whose life is otherwise untroubled. The people who receive care in the Community Heart Failure Program also suffer from drug addiction, mental illness, and are homeless or have unstable housing.
While heart failure typically affects adults over 65 whose arteries are more prone to be clogged, this program’s patients skew younger, often in their 30s-50s, with hearts whose pumping power has been reduced from the use of meth and cocaine, Smith said.
Managing heart failure in the field
To experience relief from heart failure, patients must take medications every day. Pechan and Smith’s goals are to gain patients’ trust, help them understand their condition and figure out how to take their meds on schedule. Some patients lack easy access to a pharmacy or a physical address where meds could be mailed. Some lose their meds or simply forget to take them, especially when addiction and untreated mental illness interfere.
Pechan is authorized to prescribe medication. In many cases a Harborview pharmacist will dispense the pills to her and Smith for delivery to patients. They find creative ways to help patients stay on their medications; recently they’ve had success with a small device that holds a month’s worth of pills. It has a locking lid and a timer that mechanizes the daily dispensing of doses, and a loud alarm that alerts the patient that it’s medication time.
Recognizing financial rationale
The program initially emerged from Pechan and Smith’s sense of mission to provide care for vulnerable people with heart failure. The program’s expansion, however, depended on showing that treating these patients where they live saves money.
Two U.S. healthcare policies provided financial rationale:
- Hospitals are penalized if too many Medicare patients are readmitted within 30 days of discharge for certain conditions and procedures. One of those conditions, heart failure, “is a huge medical cost by itself,” Smith said. “A single hospitalization can run into the hundreds of thousands of dollars. So, if a patient is back in the hospital within 30 days, as was the case with many of our population, there’s incentive to try something else.”
- The COVID-19 pandemic created new billable models of care that enabled Pechan and Smith to get reimbursed for out-of-hospital treatments.
“A better way is to bring heart-failure care to the people,” said Pechan. “That’s what we’re doing.”
For details about UW Medicine, please visit https://uwmedicine.org/about.