
Surgeons’ intricate handiwork focuses on sub-facial spaces
A new clinic features an eye and a sinus specialist collaborating on minimally invasive repairs for tear-duct obstruction, thyroid eye disease and orbital tumors.
Your eyes and nose are less than an inch apart, but surgeons who operate on those structures don’t routinely rub elbows. A few health conditions, however, make sense of such collaboration — like Alexandra Shapiro’s blocked tear duct, an unfortunate side effect of radiation therapy for cancer.

“In some cases, an eye surgeon would make the repair through an incision on the face, without involving an otolaryngologist (ENT),” said Dr. Aria Jafari, a sinus surgeon at UW Medicine. “In the last decade, though, endoscopic surgery has advanced and expanded our ability to go through the sinuses into the eye’s orbit and the lacrimal (tear duct) system.”
In parallel, ophthalmic surgeons also recognized that when they operated on tear ducts solo and complications arose, the problem often was scar tissue accumulating in the nose, into which the tear ducts continuously drain the fluid that keeps eyes moist.
“The role of a sinus surgeon in these cases became evident,” Jafari said.
He and Dr. Matthew Zhang, an oculoplastic surgeon at the UW Medicine Eye Institute, launched the Endoscopic Lacrimal and Orbital Clinic in spring 2022. The two surgeons collaborate on minimally invasive surgeries to treat cases of duct obstruction, thyroid eye disease and orbital tumors.
“It's a new frontier. Dr. Zhang and I have complementary skill sets and the spaces we work in lend themselves to complementary access: As you go farther back behind the eye, the space gets smaller. As you go farther back in the nose, the sinuses get bigger,” Jafari said.
The two worked in concert on July 15 to create a new path for Shapiro’s tears after her left tear duct, a pencil-lead-thin tube, was found to be beyond repair.
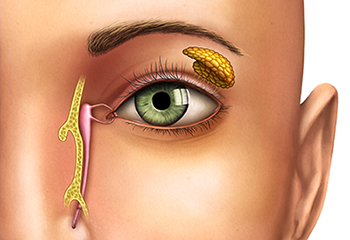
Shapiro’s original duct gradually squeezed shut after she underwent radiation to eradicate squamous cell carcinoma. The skin cancer had first been diagnosed on her left lower eyelid, for which she underwent a Mohs procedure, and then it returned to invade the infraorbital nerve on the same side, necessitating another surgery, chemotherapy and radiation.
“Somebody explained radiation as the gift that keeps on giving,” Shapiro joked this week. “My last radiation treatment ended almost two years ago, and my tear duct became noticeably blocked this past February (2022),” she said. “I was tearing continuously, and it got infected.”
In the surgery at Harborview Medical Center, Jafari approached Shapiro’s left nasal cavity with a tiny endoscope to widen the sinuses and make a new opening for tear drainage.
“In these cases, the duct that connects the tear sac to the nose is blocked,” he said. “This can be related to trauma, inflammation, a tumor or radiation therapy. Her narrowing was farther down, past her tear sac, so Dr. Zhang and I created a new passageway from the inner corner of her eye directly into the upper part of the nose.”

Shapiro’s recovery from the tear-duct procedure is going “very well,” she said. Surgery resolved the eye pressure that came with the infection, and she has had no postoperative nosebleeds. Her nose and her vision are clear, she said, and she’s glad to not be tending a scar on the tender skin beside her eye.
“I think what Dr. Jafari and Dr. Zhang did will decrease chances of infection and other problems with my eye and sinuses,” she said. “And no signs of cancer were found in the most recent MRI, CAT scan and the tissue samples. I’m very relieved and very hopeful.”
For details about UW Medicine, please visit https://uwmedicine.org/about.