
Screening key to reducing U.S. cancer deaths, panel finds
Special effort is needed to promote screening among populations who have limited access to health services, the panel said.
The United States could substantially reduce cancer deaths by closing gaps in its cancer screening programs, a presidential advisory group has concluded in a new report.
The report, “Closing the Gaps in Cancer Screening: Connecting People, Communities, and Systems to Improve Equity and Access,” was prepared by the President’s Cancer Panel, which monitors the U.S. National Cancer Program and reports to the president on barriers that might be impeding efforts to reduce cancer's impact.
The cancer death rate in the U.S. has dropped significantly over the past three decades, in large part to screening programs that detect cancers early when they are easier to treat and more likely to be cured, said Dr. Douglas E. Wood, professor and chair of surgery at the University of Washington School of Medicine. He helped organize the panel’s workshops. “Early detection not only saves lives, it makes the treatment options better, the outcomes better, and the quality of life after treatment better,” Wood said.
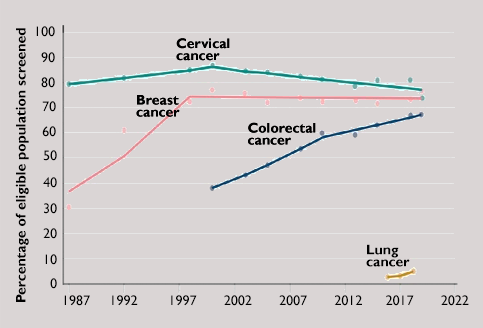
In its report, the panel focused screening programs for four cancers for which screening have been shown to be cost-effective: breast, colorectal, cervical, and lung cancers.
These programs have already had a big impact: Breast cancer death rates have fallen by about half since the 1970s, due to mammography screening and improved treatments; cervical cancer death rates have fallen 60% over roughly the same time period due to Pap smear and more recently human papillomavirus screening; and colorectal cancer incidence and mortality has fallen by about one-third, largely because of screening colonoscopy and other screening methods, such as at-home fecal tests.
Lung cancer screening is still relatively new, yet reduction in lung cancer mortality has driven record-breaking reductions in overall U.S. cancer mortality in the last three years. Clinical trials screening of high-risk individuals with low-dose computer tomography reduced lung cancer death rates by 20 percent, and United States lung cancer mortality has been dropping at a rate of 5-6% per year since lung cancer screening was implemented.
Despite these proven benefits, many people are still not getting the recommended screening, the panel noted: Rates of breast and cervical cancer screening have plateaued over the past 20 years, screening for colorectal cancer is rising but is still below target, and, according to a 2021 study, fewer than 1 in 20 of eligible smokers and ex-smokers are getting the recommended screening for lung cancer.
Wood said the low uptake of lung cancer screening is particularly concerning, because lung cancer is so common, causing almost as many cancer deaths as breast, colon, pancreas and prostate cancers combined, even a small reduction in lung cancer deaths can cause a big drop in overall cancer deaths, Wood said. “The number of lung cancer deaths is so big, even a modest increase in early detection would move the needle a lot,” he said.
The panel calls for both public and private health providers and insurers to pursue four goals to improve screening: one, improve communication efforts especially those targeting groups among whom cancer screening rates are low; two, facilitate more equitable access to screening by expanding community outreach programs and increasing access to tests that can be performed at home; three, change payment rules to broaden the types of staff who can provide counseling and participate in required shared-decision making; and, four, develop integrated electronic health information systems that will facilitate screening.
This news item was written by Michael McCarthy.
For details about UW Medicine, please see our About page.
Topics:cancermammography