
Program will bring antidepression therapies to dialysis units
Removing dosing guidance from a guideline summary takes a valuable tool from prescribers, says Dr. Mark Sullivan and pain-medicine colleagues.Media Contact: Brian Donohue - 206-534-7856, bdonohue@uw.edu
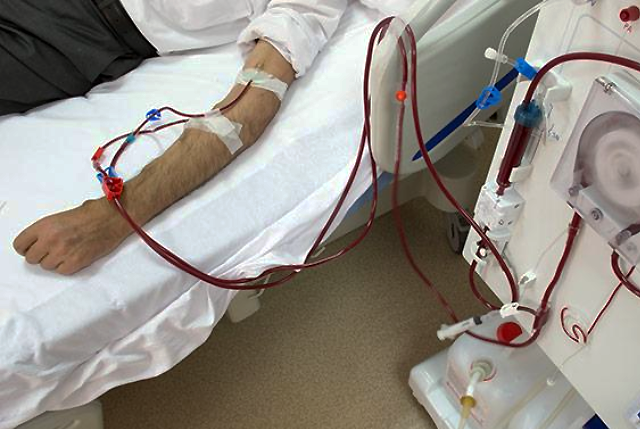
Telling a patient that their kidneys have failed and that they need to go on dialysis is tantamount to saying their life is no longer their own, Dr. Raj Mehrotra says.
“Kidney failure involves a series of losses. Not simply a potential loss of years of life, but also lifestyle: Your diet must change. You may have to quit your job. You’ll have less time to travel and do activities that you enjoy. You’ll have a medication regimen of 19 pills a day, on average,” he said.
Now imagine how much harder these life changes would be, he added, for someone who is managing depression, too.
That is the backdrop to a just-announced $2.1 million grant to develop a clinical-delivery program for two treatments found effective at improving mental health among people on dialysis. This program would make the antidepressant drug sertraline and cognitive behavioral therapy available to more than 8,300 people at Satellite Healthcare dialysis centers in California, Texas, Georgia and Tennessee.
Funding comes from the Patient-Centered Outcomes Research Institute (PCORI), an independent nonprofit. Mehrotra, head of nephrology at the University of Washington School of Medicine, is the grant’s principal investigator.
He led the study published in 2019 that showed both therapies, randomly assigned to dialysis patients over 12 weeks, similarly reduced depression — though participants who received the drug therapy experienced more side effects.
“The goal of that study was to generate information that patients and physicians could use to decide, if they have depression, which treatment makes sense,” Mehrotra said.
It’s an ambitious undertaking to transform those findings into a viable therapy-delivery program in 87 dialysis centers across four states. The aim is to offer the choice of therapies to 8,350 people who currently receive care at those centers.
“The main question for us to answer is: Can we reconfigure the systems and staff at dialysis centers to make both of those treatments available? Because currently, neither is available consistently for patients undergoing long-term dialysis in the United States; a patient has to go to a third party to get those treatments.”
Before any new patients are even screened for depression, electronic medical record systems must be revamped to capture information about the treatments and outcomes. Staff social workers and nephrologists in the participating dialysis units will need to be trained to manage depression.
“In our plan, the social workers will deliver cognitive behavioral therapy via telehealth,” Mehrotra said. “The sertraline prescriptions need to be written by the unit nephrologist, and one challenge may be the willingness of the nephrologists to engage in treating a psychiatric condition.”
The researchers will scrutinize the program’s effectiveness — at getting patients screened, at ensuring that patients with depression are offered both therapies, and that obstacles to therapy are overcome. For example, a patient who does not have access to high-speed computer data at home should still be able to opt for CBT via telehealth and receive it at their dialysis clinic, Mehrotra said.
“And then, in people who get treatment, does their depression get better? That continues to be important to demonstrate in the hope of scaling this program to other dialysis centers,” he added.
For details about UW Medicine, please see our About page.