
Doctors should be on the lookout for perinatal depression
Left untreated, the condition can hinder bonding and healthy attachment between mother and child, a report states.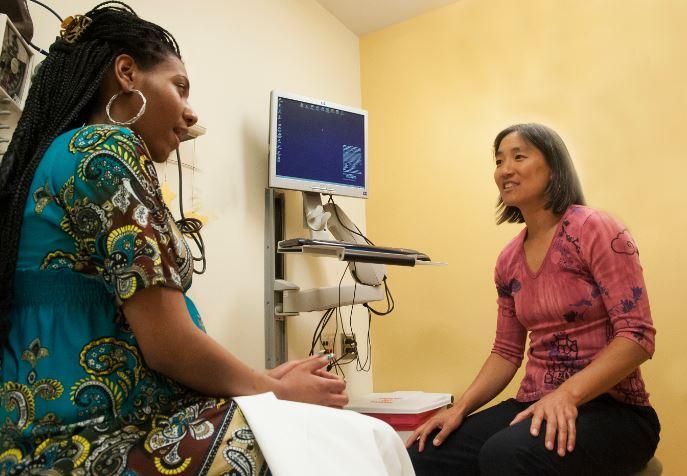
In a policy statement this month, the American Academy of Pediatrics urged pediatric healthcare providers to watch for signs of perinatal depression in the mothers of their infant patients. The statement and accompanying technical report will be published in the January 2019 issue of Pediatrics.
“This is a welcome update of clinical guidance,” said Ian Bennett, a professor of family medicine and of psychiatry and behavioral sciences at the University of Washington School of Medicine. “The medical profession used to think that being pregnant protected a mother from depression. Now we know that most women who have postpartum depression actually were already depressed during pregnancy,” Bennett said. “There is a real blind spot in our society regarding perinatal depression."

An estimated 50 percent of women who are depressed during and after pregnancy go undiagnosed and untreated, according to research cited in the report. Left untreated, perinatal depression can hinder bonding, distort perception of the infant’s behavior, and impair the mother’s attention and judgment concerning safety.
After a baby is born, there is an expectation that moms will become “warrior women” who deftly deal with motherhood, jobs, family, and society in general, he noted.
Women are twice as likely in their reproductive years (ages 15 to 45 ) to experience bouts of major depression, he said. In this same population, about 12 percent to 15 percent will experience some level of depression -- about twice the incidence of males in the same age range.
These statistics do not suggest that depression cannot be managed, said Bennett. He and colleagues have been working with UW Neighborhood Clinics physicians to recognize depression in pregnant women and those who bring babies for checkups.
For several years, UW Medicine's primary-care network has used an evidence-based collaborative care model for depression. The UW-developed model consists of a provider team at each clinic. A care manager reviews patients with depression weekly with a psychiatric consultant to assess treatment plans and support the primary-care and obstetric providers working with these patients.
Four of the clinics are taking part in an NIH study about recognizing perinatal depression in patients and using face-to-face and remote-care models. The study is set to be completed in 2021.
Bennett encourages providers to raise the issue directly. “Usually there is some concern by the physicians that they might annoy or offend the patients by asking them about depression,” he said. “But in fact, pregnant and parenting women are very receptive to someone asking about this topic.”
Washington providers who have questions about caring for a pregnant or new mom with a mental health and/or substance abuse problem can call the UW PAL for Moms line (877-PAL4MOM; 877-725-4666). PAL for Moms is a free consultation line staffed by UW Medicine psychiatrists where providers can receive advice on pregnancy loss, infertility, depression, anxiety, risks of psychiatric medications, non-medication treatments and more.
UW Medicine psychiatrists can also provide a free, in-person overview of best practices for depression screening for clinics as well as how best to follow up in the perinatal period. Visit https://www.mcmh.uw.edu or email mcmh@uw.edu to learn more.
For more information or to interview Dr. Bennett, contact Media Relations Manager Barbara Clements at 206.221.6706 or bac60@uw.edu.
For details about UW Medicine, please see our About page.