
Diabetic retinopathy diagnoses seen nearing 10M in U.S.
Authors say resources can be allocated based on this first analysis to estimate the number of people of all ages with the vision disease.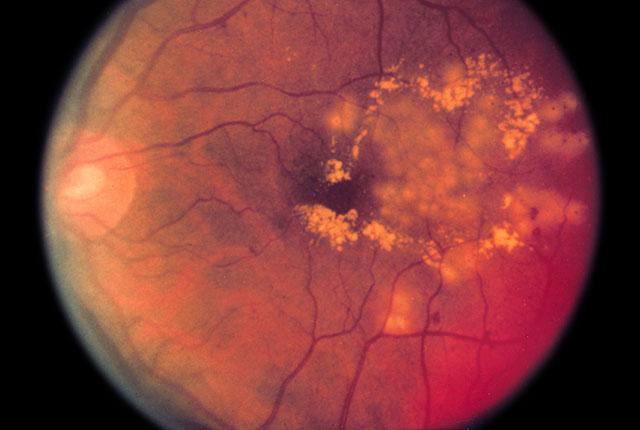
For the first time, a comprehensive statistical analysis has enabled researchers to estimate the number of Americans of all ages living with diabetic retinopathy, and the number’s not pretty.
The study conducted by researchers at the Centers for Disease Control and Prevention, the University of Washington School of Medicine and NORC (formerly called the National Opinion Research Center) at the University of Chicago indicates that 9.6 million people had diabetic retinopathy in 2021. That’s about 30 percent higher than the previous research had predicted. Of those, 1.8 million have vision-threatening disease.
The simple takeaway?
“This is common,” said Abraham Flaxman, one of three UW co-authors. “About 1 out of 4 of the people who are living with diabetes, at least age 40 and older, have diabetic retinopathy.”
Diabetes affects more than 37 million Americans, a count that grows with obesity and poor nutrition. Diabetic retinopathy occurs when high blood sugar damages small blood vessels in the retina. This can lead to vision loss.
The study was published in June in JAMA Ophthalmology. Researchers used data from the CDC’s Vision and Eye Health Surveillance System, which collated information from the National Health and Nutrition Examination Survey, Medicare and private insurance claims, and studies of adult eye disease and diabetes in youth.
Flaxman is an associate professor in global health and health metrics sciences, and an adjunct associate professor of computer science and engineering. Dr. Aaron Lee from UW Medicine ophthalmology and Zeb Burke-Conte at the Institute for Health Metrics and Evaluation also contributed to the research.
The authors’ major challenge was that, in 2008, the CDC stopped including direct measurements of diabetic retinopathy in its flagship National Health and Nutrition Examination Survey, Flaxman said.
“We have great measurements up until 2008 and then we have a lot of filling in the gaps to do,” he said. “What this study is really all about is taking all the great measurements that are now out of date, all the partial measurements that capture some important parts of the story that have come out since then, and putting them all together.
“It’s been a long time and diabetes is something that has been changing over 15 years.”
A map generated for the study shows diabetic retinopathy hot spots around the nation. The investigators hope the research can be used to allocate public health resources and interventions to communities at high risk.
“A limitation of this work is that unfortunately this is not the kind of analysis that says why,” Flaxman said. Reasons might include better diagnostic abilities and greater access to healthcare, meaning patients are counted at a higher rate than in other states. Or it might mean that something inscrutable is going on with vision and eye care here that we can’t yet identify.
Knowing where to look is the first step to finding meaningful context, Flaxman said. The new analysis is a reminder of how important baseline analyses are for the greater good.
“I hope the takeaway from this is there's no substitute for really going out and gathering the data,” Flaxman said. “And it seems like CDC is really on board for that. And they, I hope, will be renewing this direct measurement in their regular NHANES study. That will just be a huge addition to what we know and what we can say about vision and eye health.”
This news item was written by Chris Talbott, 206-543-7129, talbottc@uw.edu.
For details about UW Medicine, please visit https://uwmedicine.org/about.