
App for serious mental illness starts clinic-training phase
The phone-based technology is "the closest thing to a therapist in patients’ pockets," says its project lead in psychiatry at UW Medicine.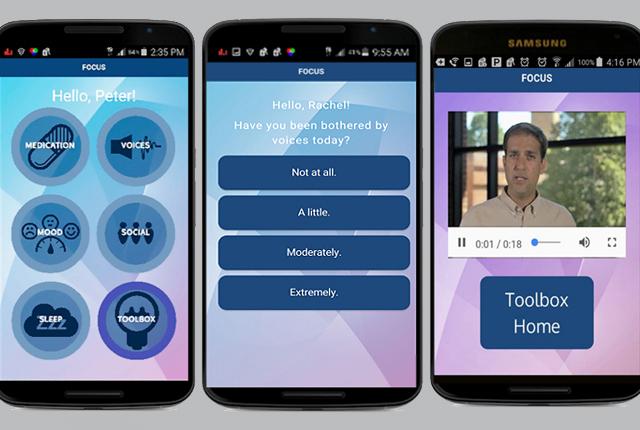
UW researchers this week were awarded $1.8 million to bring a mental health smartphone app into real world practice.
The Patient-Centered Outcomes Research Institute announced funding for the FOCUS app, which has shown promise as a supportive therapy for people who have serious mental illness such as schizophrenia and bipolar disorder.
“It’s the closest thing to a therapist in patients’ pockets,” said Dror Ben-Zeev, a professor of psychiatry and behavioral sciences at the University of Washington School of Medicine. He has guided the app's development through early user studies, the most recent of which showed that patients found the digital therapy more engaging than a scheduled trip to the clinic — the far more resource-intensive conventional care.

The next step for FOCUS involves rolling out a system aimed at teaching clinicians how to engage patients to use the app confidently and how to get the most information from patients’ use.
“We demonstrated that FOCUS is clinically potent in several studies, but to move this from academic research to real-world practice, we need an implementation approach that includes digital trainings for clinicians who are not used to mental health apps. This will support their journey as digital health adopters, which is a daunting task for some. We’re creating evergreen materials so any clinician will be able to get FOCUS up and running with their patients quickly,” Ben-Zeev said.
Part of the study is to understand how different clinic staff might need different information upfront about FOCUS to introduce it in a compelling way to their colleagues.
“It could be frontline clinicians or admin support people or team leaders, so we need to ensure that we finely tune the information that helps FOCUS make the greatest impact it can,” Ben-Zeev said.
The FOCUS app has written and video content adapted from in-person, evidence-based interventions. Its treatment domains address:
- auditory hallucinations (“hearing voices”)
- mood problems (typically depression and anxiety)
- sleep
- social functioning such as social skills training or paranoia
- medication use (reminders and information to examine counter-therapeutic beliefs that people might have about their medications)
Ben-Zeev described a hypothetical scenario of an app-driven intervention with a patient who is hearing voices that predict an ominous future.
“This is a dysfunctional belief related to the predictive power of voices. FOCUS helps its users understand that voices make mistakes all the time and suggest that the patient test the voices by asking them to predict the color of the next three cars that come into view. It's a tactical suggestion that leverages something in their immediate environment,” he said. “The idea is, if the voice’s prediction is wrong, that can open the user to wonder what else might the voices be getting wrong, hopefully diminishing the voices’ power.”
The app’s 24/7 availability is a huge advantage for patients who may have mental health needs outside clinic hours and who otherwise might need to wait several weeks or more to address an episode in a clinic environment.
Moreover, many patients with serious mental illness receive services at community mental health centers. These facilities often are under-resourced and less able to provide continuity of care due to high turnover rates among their staff. FOCUS can provide continuity of care as clinical staffing ebbs and flows, Ben-Zeev said.
The study will be conducted in collaboration with the adult outpatient programs at community mental health agencies in New Hampshire and Missouri that care for people with serious mental illness: The Mental Health Center of Greater Manchester, Community Partners New Hampshire, and Places for People in St. Louis City.
Related: BRiTE Center (FOCUS developers)
For details about UW Medicine, please see our About page.