
App encourages clinical talks about fertility, reproduction
Data shows that 14% of primary-care visits among women of reproductive age include contraceptive and reproductive counseling.
For many women, it is difficult to share feelings about becoming pregnant with their healthcare providers. That can be particularly true if you’re a veteran.
“The lack of open and respectful conversations about people’s reproductive hopes and goals in clinical settings makes it harder for them to get the care they need,” says Dr. Lisa Callegari. She's an associate professor of obstetrics and gynecology at the University of Washington School of Medicine and a researcher at the VA Puget Sound Health Care System.
Callegari was lead author of a paper recently published in the Journal of General Internal Medicine. It examined the efficacy of patients using a smartphone app to address fertility and birth-control concerns before an office visit with her doctor or primary-care provider.
National data indicates that only 14% of the U.S. primary-care visits with non-pregnant women of reproductive age includes counseling about contraception and pregnancy. In a VA study of women who could become pregnant, those conversations were a bit more frequent (38%) but still low, the report added.
Female veterans face additional hurdles in talking about their reproductive goals with VA providers. For one, women are a numeric minority in a healthcare system originally built for men, Callegari noted. Research led by Callegari last year showed that female veterans often don’t realize that VA offers pregnancy care and birth control, and many of those patients expressed concern that their reproductive needs may not be a priority for VA clinicians.
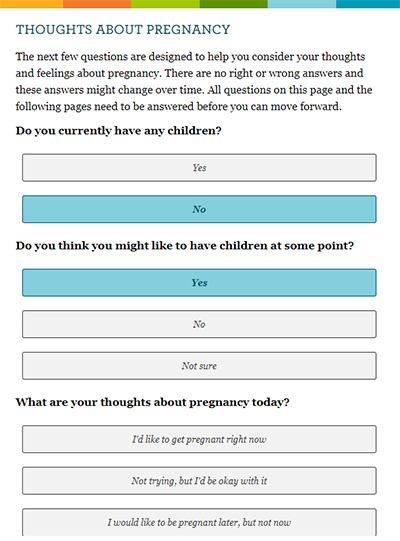
Callegari and her team have set out to shift this dynamic. They developed MyPath, a patient-facing, internet-based tool designed to encourage patients’ to share individual goals, preferences and needs during clinical discussions about pregnancy and birth control.
“We knew there were apps out there to help people discuss their birth-control preferences and options with providers, but none that started with questions about pregnancy desires or goals, or helped people to also get information about fertility or optimizing health before desired pregnancies,” she explained.

The MyPath tool takes the user through a series of questions about whether they want to become pregnant, and if so, when. It offers modules about fertility, health and pregnancy, and birth-control methods. MyPath generates a summary page of users’ interactions, which can be brought to clinic isits.
With a small, VA-funded study of 58 women veterans, Callegari’s team analyzed whether the use of MyPath on an iPad before clinic visits would change the direction of in-clinic conversations. The researchers found that MyPath was highly acceptable among participants, helped them to feel prepared going into visits, and boosted their ability to communicate. About 93% of users reported that they discussed their reproductive needs with their doctor, versus 68% in a control group.
Primary-care providers reported that MyPath did not significantly increase their workload and most felt it helped in counseling patients, the findings stated.
Callegari’s team recently received funding to test MyPath in a randomized controlled trial at seven VA sites across the country, including Puget Sound. The study started in January and will be completed in three years. The study will randomize 30 primary-care providers and 450 patients to receive MyPath prior to scheduled visits or receive usual care without the app.
The trial will offer MyPath to patients through a a linked text message. The researchers hope that this delivery tactic, which is low-cost and highly scalable, will make it easier to implement MyPath widely if it is found to be effective.
Although MyPath was developed in the VA system, Callegari is partnering with researchers outside of the VA to explore the technology's use in other settings, including in health clinics in Indiana and substance abuse clinics in Pittsburgh. Callegari also plans to study whether MyPath is as effective across populations who experience racism or discrimination in healthcare settings, including women of color and LGBTQ individuals.
“We’re hoping that testing MyPath in a variety of settings and populations, with a focus on marginalized people who face the biggest challenges in receiving high quality reproductive health care, will best position us to make a positive impact,” she said.
For details about UW Medicine, please visit https://uwmedicine.org/about.