
Why is COVID-19 more severe in men and elders?
SARS-CoV-2 usually triggers a strong immune response, but less so in men and people over 60.Media Contact: Susan Gregg, 206.390.3226, sghanson@uw.edu
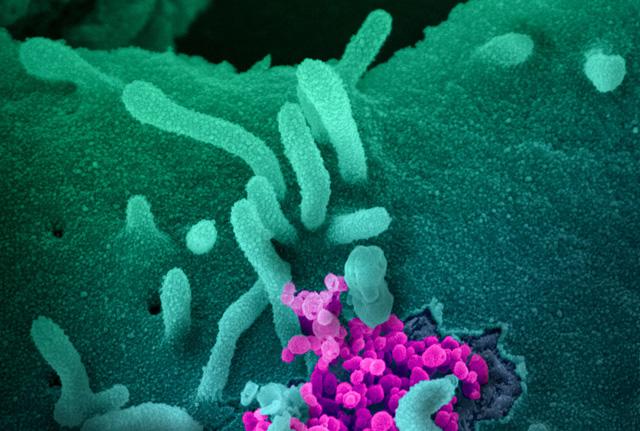
The immune system usually mounts a strong immune response to infection by SARS-CoV-2, the virus that causes COVID-19. That defensive response, however, appears to be weaker in men and people over the age of 60, a study led by researchers at the University of Washington School of Medicine in Seattle has found.
“There were some early studies that suggested that there was a fairly weak antiviral response shortly after infection, but we found a very robust immune response in patients at the time of symptom onset,” said lead author Nicole Lieberman. “But differences in the immune response in older individuals and men may contribute to the greater severity and higher mortality we see in these groups.”
Lieberman is a research scientist in the laboratory of Alex Greninger. He is an assistant professor in the department of Laboratory Medicine and Pathology at the University of Washington School of Medicine and head of the project. The results of the study appear in the open-access journal PLOS Biology. Here is the paper.
In the study, the researchers compared samples swabbed from the noses and throats of 430 people who were infected with SARS-CoV-2 and 54 people who were not. They also worked with colleagues at Columbia University Medical Center in New York City and University of Texas Medical Branch, Galveston, Texas. These groups have developed techniques to infect cells in culture to track changes in the immune response over time.
To assess immune responses the researchers analyzed the RNA in the samples. Because the SARS-CoV-2 stores its genetic instructions in RNA, levels of viral RNA in the samples revealed the amount of virus, or “viral load,” an indicator of the severity of infection. In human cells. On the other hand, RNA reveals which proteins the cells are producing in response to the infection. That’s because, for the instructions for synthesizing proteins encoded in the DNA of genes to be “read” by the cells, the code must first be copied, into RNA. As a result, analyzing the RNA transcriptsin a sample can show which genes are being dialed up in response to the infection and which are being dialed down. This sort of analysis can reveal what sort of immune counterattack the cells are mounting against the virus.
The researchers found that the viral load in these patients was high, but also that SARS-CoV-2 triggers a strong antiviral response. This includes up-regulation of genes for a number of antiviral factors that activate the cells’ defenses against viral invaders. It also includes chemical signals that summon immune cells to fight the infection, such as interferons and chemokines.
“The viral load with SARS-CoV-2 infection is one of the highest seen,” Greninger said. “But the immune response is very strong, and the higher the viral load, the stronger the response.”
However, in older individuals over age 60, infection did not activate genes to summon virus-fighting cells called cytotoxic T cells and natural killer cells that are some of the body’s the most effective antiviral weapons.
“The older patients activate a weaker immune response – like a singer that just can’t hit the high notes anymore,” Greninger said.
The researchers also found that men mounted a less vigorous response compared to women. The males produced lower levels of transcripts of some anti-viral proteins, and pumped out some proteins that put a damper on the immune response.
“In men we’re seeing an up-regulation of signals that turn off the immune system,” Lieberman said. “It’s speculation, but it appears as though some men may throttle back their immune system too soon before mounting an effective response to infection.”
This work was supported by National Institutes of Health (AI146980, AI121349, and NS091263) and the Department of Laboratory Medicine and Pathology at the UW School of Medicine.
For details about UW Medicine, please see our About page.