
Study questions reliability of diagnostic tests for herpes
Up to half of those screened for genital herpes may be incorrectly told they are infectedMedia Contact: Brian Donohue: 206.543.7856; bdonohue@uw.edu
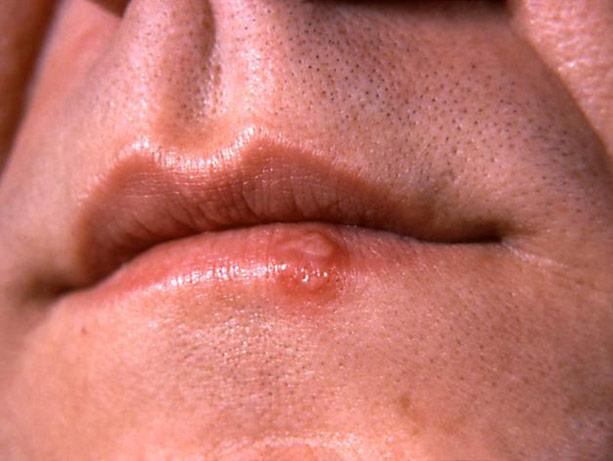
Tests commonly used to diagnose oral and genital herpes are often unreliable, missing some cases of infection and, in others, identifying an infection that does not exist, say researchers at the University of Washington School of Medicine.

In nearly half of patients with commercial test results indicating that they were infected with the most common cause of recurrent genital herpes, herpes simplex virus 2 (HSV-2), a subsequent test showed that the initial diagnosis was incorrect, the researchers report in a paper published today in the journal Sexually Transmitted Diseases.
The high rate of false-positive HSV-2 tests was particularly troubling, said Dr. Anna Wald, who led the research.
“These tests aren’t as good as they ought to be, given that they are used to diagnose someone with a chronic, lifelong sexually transmitted disease.” Wald directs UW’s Virology Research Clinic and is a professor of medicine, epidemiology, and laboratory medicine.
The investigators examined results from FDA-approved tests used to diagnose HSV-2 and herpes simplex virus type 1 (HSV-1), the most common cause of cold sores.
These tests, called enzyme-linked immunoassays, detect the presence of antibodies to the herpes simplex viruses in a person’s blood. When the antibodies are detected, the test is positive, meaning that the person is infected by the virus. No detected antibodies indicates no infection.
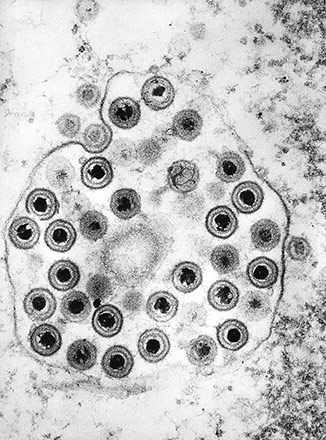
To assess the tests’ reliability, the UW researchers reviewed the charts of 864 patients from a private sexually transmitted disease clinic in Portland, Oregon, who had been tested for herpes simplex virus antibodies with one of the commercially available immunoassays and who then sought a follow-up confirmation test developed in the UW laboratories. This test, called the UW Western Blot is considered a highly accurate, “gold standard” test.
For HSV-1, the researchers found that, among the 278 people whose immunoassay registered as positive, 255 were confirmed infected by blot test, suggesting that a positive immunoassay result for HSV-1 is likely reliable. However, the immunoassay missed about 30 percent of those whose HSV-1 infection was positively identified with the blot test.
More troubling were the antibody test results for HSV-2. Of the 381 patients who tested positively, only 50.7 percent were confirmed as infected with the blot test.
“These findings indicate that if you didn’t have signs and symptoms of genital herpes and were diagnosed by an (immunoassay antibody) test alone and had a low positive index value, there’s a 50-50 chance the test was wrong,” Wald said. “In that case, you should get a confirmatory test.”
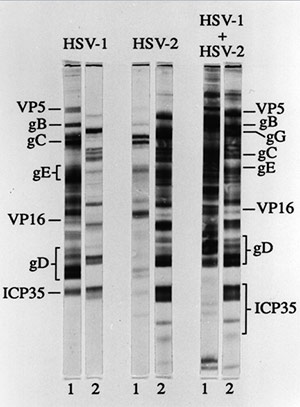
“We know that lab tests are not perfect, but this margin of error for both HSV-1 and HSV-2 is not acceptable. Clearly we need better tests,” Wald said.
Current guidelines recommend antibody tests for HSV-1 or HSV-2 for people who have partners with genital herpes, who have atypical symptoms that might be genital herpes, or who have been diagnosed with herpes by visual exam only. General screening of people who have no symptoms is not recommended.
“People often request HSV tests when they are concerned about their sexual health. People about to start a new relationship want to know what they bring to the bedroom, and since genital herpes is a common STD, and often asymptomatic, it seems reasonable to want to be tested for it,” Wald said.
Federal regulators have proposed limiting lab testing to commercial tests approved by the U.S. Food and Drug Administration – a change that Wald opposes.
“Many laboratories, especially academic laboratories, have developed and validated their own tests,” she said. “In case of testing for HSV, limiting testing to FDA-approved tests will deny patients access to these more reliable tests.”
Study co-authors include nurse practitioner Terri Warren, in whose clinic the study was based, and Dr. Keith Jerome, head of the UW Virology Division, in whose lab the Western blot test is performed.
For details about UW Medicine, please see our About page.
Topics:diagnosticsherpes