
Seattle team pivotal to FDA OK on drug for rare skin cancer
UW Medicine and Fred Hutch had key roles in clinical trial of immunotherapy option for often-lethal Merkel cell cancer.Media Contact:
- UW Medicine: Brian Donohue – bdonohue@uw.edu, 206.543.7856
- Fred Hutch: Molly McElroy – mwmcelro@fredhutch.org, 206.667.6651
An immunotherapy clinical trial based in Seattle, among other U.S. sites, was pivotal to the Dec. 19 approval by the Food and Drug Administration of the drug pembrolizumab (Keytruda) to treat Merkel cell carcinoma, a rare and often fatal skin cancer.
The FDA’s accelerated approval of the drug was based on findings from a trial of 50 patients at 13 clinical sites across the United States, including 12 patients, the largest cohort, in Seattle. The trial was initiated in 2014 by the Cancer Immunotherapy Trials Network (CITN), which is based at the Fred Hutchinson Cancer Research Center, and was sponsored by the National Cancer Institute.

“This is an approval based on the strength of one trial, which is unusual,” said Paul Nghiem, the trial’s principal investigator. He is professor and chair of dermatology at the University of Washington School of Medicine.
The multicenter, Phase II trial involved patients with recurrent locally advanced or metastatic Merkel cell carcinoma who had not received previous systemic therapy for their disease. They received 2 mg/kg of pembrolizumab via intravenous infusion every three weeks.
Among the 50 patients, the drug’s overall response rate was 56 percent – about the same as standard chemotherapy treatment, Nghiem said. But pembrolizumab helped a significant subset of patients survive much longer than would be likely with chemotherapy: Among those who responded favorably to the therapy, 96 percent responded for durations of greater than six months and 54 percent for durations of greater than 12 months.
In striking contrast, historical data show that only about 10 percent of patients with advanced MCC who received first-line chemotherapy would have a comparable response; most patients’ responses lasted only weeks or a few months.
“We are extremely pleased that the results of this CITN trial have been so positive,” said Martin A. “Mac” Cheever, CITN director and an immunotherapy scientist at Fred Hutch.
Those results compelled the FDA to fast-track its consideration of pembrolizumab for MCC.

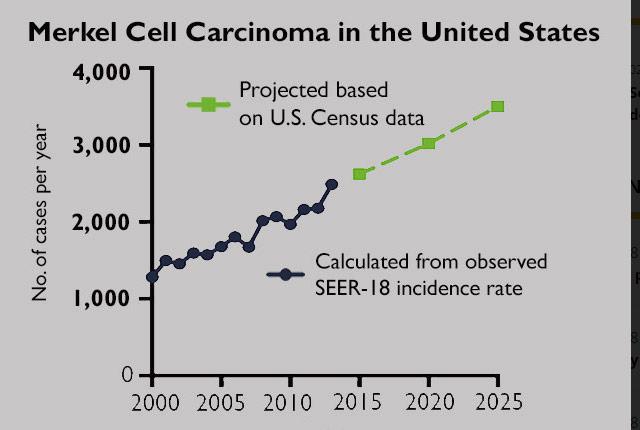
Merkel cell carcinoma has long been an orphan disease, drawing little attention from pharmaceutical companies because of its low incidence – only about 2,500 cases a year in the United States, according to the American Cancer Society. In the majority of cases, the driving factor is a virus that is often present on normal skin. A minority of cases stem from skin exposure to ultraviolet light.
The cancer kills about half of those who develop it.
The trial therapy, manufactured by Merck, is designed to act by reinvigorating cells of the immune system that can normally attack the cancer, but are suppressed through a protein called PD1. Pembrolizumab blocks the PD1 effect and can release an immune response.
The national guidelines for MCC have changed based on this trial and others.
“Chemotherapy was the major intervention for advanced Merkel cell carcinoma. Now chemotherapy is disfavored and immunotherapy is the main approach. That all happened in a two-year window, which is really fast for a complete flip of options,” Nghiem said.
He credited Cheever and the CITN for persistence with the National Cancer Institute and Merck to support a clinical trial.
The next steps, he suggested, are to better understand why some patients respond to immunotherapy and others don’t. “By learning more about the basic biology and the immune response to Merkel cell cancer, we hope to develop even more effective therapies.”
Related links:
For details about UW Medicine, please visit https://uwmedicine.org/about.