
How much time for surgery? Researchers create model
Of all the data captured, the greatest variability was between surgeons, the study published in the Journal of the American College of Surgeons, showed.Media Contact: Bobbi Nodell, bnodell@uw.edu, 206.543.7129
Operating rooms are a precious resource. They may account for 50 percent of a hospital’s revenues and cost as much as $80 a minute. But figuring out how much time to allot for a surgery is a challenge every hospital faces.
“OR scheduling is a $5 billion problem. To optimize the OR, you have to answer a fundamental question: How long does each surgery take?” said co-lead author Rajeev Saxena, an anesthesiology resident at the University of Washington School of Medicine. “Underutilization means fewer patients get surgical care and the hospital has excess capacity. Overutilization results in cancelled operations and overtime expenses.”
To try to improve the prediction of surgical-case duration, Saxena, in collaboration with physicians in surgery and anesthesia, scientists, and informatics experts inside and outside University of Washington, created machine-learning models for each surgical specialty and for individual surgeons.
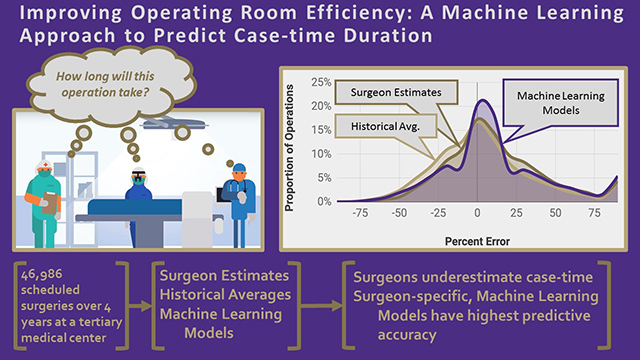
Their study, “Improving operating room efficiency: A machine-learning approach to predict case-time duration,” was published July 18 in the Journal of the American College of Surgeons.
The researchers collected data from over 45,000 surgeries over four years performed by 92 surgeons. Their surgeon-specific models were able to improve accuracy from 30 percent (based on a surgeon’s estimate) to 39 percent. Among the top-third of surgeons, accuracy improved to more than 50 percent.
As more data is inputted, the model will improve over time, noted co-lead author Matthew Bartek, a general surgery chief resident at the University of Washington Medical Center.
“If we can improve the data, we can zero in on more accurate estimates,” Bartek said. “This is just the first step.”
To create their estimates, researchers gathered data from multiple electronic medical records on the patient, the type of surgery, the surgery personnel, and the surgery scheduling information. Only preoperative data was used.
Of all the data captured, the greatest variability was between surgeons.
“Each surgeon has a unique approach to an operation and this data confirmed it,” said senior author Bala Nair, former director of a UW School of Medicine technical center that looked at improving care through informatics and technology solutions.
“This work is bringing operating rooms into the 21st century by applying modern data science methods to improve operations,” he said.
“For years, operating rooms have been relying on surgeon’s estimates for operating times. But surgeons usually greatly underestimate the time of procedures,” said senior author John Lang, clinical director of operative and perioperative operations at UW Medicine.
Lang said two hospitals in the UW Medicine system are rated by the Medicare Case Mix Index highly for complex surgeries. UW Medical Center is rated No. 3 and Harborview Medical Center is rated No. 13. Because of this, accurate prediction of surgical case duration is especially challenging and impactful.
Said Saxena: “You can change an entire organizational culture by taking a data-forward approach and engaging key stakeholders."
Other collaborators on this study included Stuart Solomon, an anesthesiologist at UW Medicine and Christine Fong, an informatics engineer at UW Medicine. The work was done in collaboration with Perimatics, a Bellevue, Wash-based data science company.
For details about UW Medicine, please see our About page.
Topics:surgery