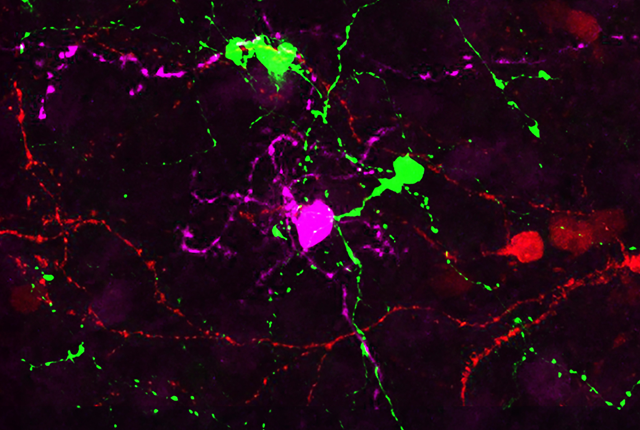
Ganglion cells created in mice in bid to fix diseased eyes
Media Contact: Chris Talbott, 206-543-7129, talbottc@uw.edu
While fish, reptiles and even some birds can regenerate damaged brain, eye and spinal cord cells, mammals cannot. For the first time, non-neuronal cells have been induced to mimic specific ganglion cells in the eyes of mice.
The hope is that one day this advance could create a new path to treat a variety of neurodegenerative diseases, including glaucoma, macular degeneration and Parkinson’s disease.
A UW Medicine team led by Tom Reh, professor of biological structure at the University of Washington School of Medicine, had previously shown that neurons could be coaxed from glial cells in the retinal tissue of mice. Now they’ve refined the process to produce specific cells.
“We could only make primarily one type of neuron — the bipolar neuron,” Reh said. “And like we would say at the time, ‘We can make the one type of neuron that nobody loses to disease.’ So while it was pretty amazing, it was also not super clinically relevant. Since that time, we've been trying to figure out whether we can do further tinkering with this process in mammals and see if we can expand that repertoire of types of neurons that can be regenerated.”
A paper describing the results appeared Nov. 23 in Science Advances. Postdoctoral researcher Levi Todd and graduate student Wesley Jenkins in Reh’s lab are the paper’s co-lead authors.
Over the last three years, the researchers have studied proteins called transcription factors in vertebrates, such as zebrafish, that have regenerative abilities. Transcription factors are proteins that bind to DNA and regulate the activity of genes. This, in turn, controls the production of proteins that determine a cell’s structure and function.
Previously the team learned how to use the transcription factors to return the glia to a more primitive state known as a progenitor cell. Further treatment then can push the progenitor cell in other directions.
In this case, they tried to create retinal ganglion cells — the type lost to glaucoma.
This approach “could potentially have really wide applicability because the principle is you get the ball rolling by making your glia into a progenitor-like cell, but now you don't just let that cell do whatever it wants,” Reh said. “You control it and channel it down specific developmental trajectories. I think it's going to be generally applicable in other areas of brain repair and spinal repair.”
Todd said the researchers are making a “playbook” of transcription factors.
“Usually when you have a disease like a Parkinson's, dopamine neurons die,” he said. “If you have glaucoma, ganglion cells die. We want to figure out how to make glia into that specific type of neuron.”
The team has received grant funding from the Foundation Fighting Blindness to study whether the same process will work in human and monkey eye tissue. Reh said the work is underway and that other teams are also pursuing similar research.
“I hope we can show in three years that it works in monkeys and humans,” Reh said. "I think we are pioneering this approach for the field, and others are coming in now. It won't surprise me if we're not the first ones to find the magic mix for cones or the magic mix for some particular subtype of ganglion cell. But I think we set the paradigm of how you can move forward on this and how you can now get better at it and refine it.”
Computational biologist Connor Finkbeiner, postdoctoral fellow Marcus J. Hooper, undergraduate researcher Phoebe C. Donaldson, postdoctoral researchers Marina Pavlou, Juliette Wohlschlegel and Norianne Ingram, and Fred Rieke, professor of physiology and biophysics, also participated in the research.
This project was funded by the National Institutes for Health (NEI R01EY021482, K99EY033402), the Gilbert Family Foundation’s Vision Restoration Initiative, a Washington Research Foundation fellowship, an International Retina Research Foundation fellowship and a Mary Gates undergraduate scholarship.
The authors’ conflict of interest statement is available in the paper or by contacting UW Medicine media relations.
Broadcast-ready media resources:
For social media/embedding:
For details about UW Medicine, please visit https://uwmedicine.org/about.