
Tomosynthesis bests mammography in community practice
A study showed that digital 3D breast tomosynthesis leads to better cancer-screening performance than 2D mammography.Media Contact: Brian Donohue - 206-543-7856, bdonohue@uw.edu
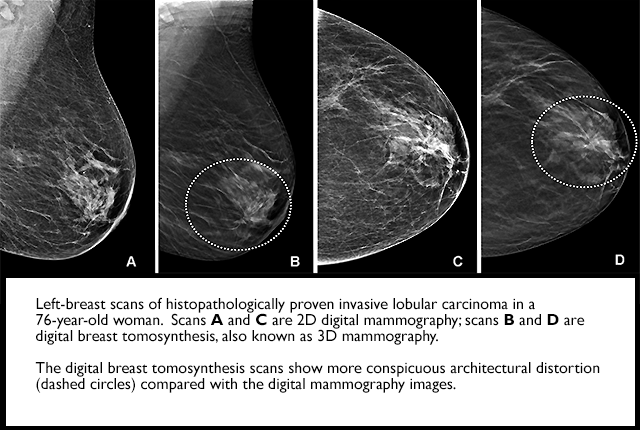
Researchers have found that digital breast tomosynthesis (DBT) has improved breast-cancer screening performance in community practice and identifies more invasive cancers, compared with digital mammography. In addition, radiologists’ interpretive performance has improved with DBT.
The findings were published April 11 in Radiology.
“Our study demonstrated that more radiologists in U.S. community practice are meeting recommended performance standards with digital breast tomosynthesis than they did with digital mammography,” said Dr. Christoph Lee, the lead author and a professor of radiology at the University of Washington School of Medicine in Seattle. “This is good news for women and breast cancer screening, as digital breast tomosynthesis has quickly become the most popular breast cancer screening modality in the U.S.”
After gaining Food and Drug Administration approval in 2011, DBT was rapidly adopted in the United States. As of September 2022, 84% of all U.S. mammography screening facilities had DBT units.
Breast-cancer mortality reduction from routine screening is contingent upon radiologists’interpretive performance. Since the Mammography Quality Standards Act emerged in 1992, screening facilities and interpreting radiologists have been required to meet minimum quality standards. Starting in 2006, the Breast Cancer Surveillance Consortium (BCSC) has published screening-performance benchmarks. The BCSC is a collaborative network of breast imaging registries conducting research to assess and improve the delivery and quality of breast cancer screening and related patient outcomes.
To establish performance benchmarks for DBT screening and evaluate performance trends over time in U.S. community practices, the research team analyzed DBT screening exams from five regional BCSC registries between 2011 and 2018.
Performance measures included abnormal interpretation rate, cancer detection rate, sensitivity, specificity and false-negative rate.
Compared with BCSC digital mammography screening exams from the same time period and previously published BCSC and National Mammography Database performance benchmarks, all performance measures were higher for DBT except sensitivity and false-negative rate, which were similar to concurrent and prior digital mammography performance measures.
“Radiologists appear to perform better with digital breast tomosynthesis and have higher accuracy on screening 3D mammograms than 2D mammograms across U.S. practices,” Lee noted. “As this becomes the mainstay screening modality, we hope to see improved screening outcomes for women.”
A total of 896,101 women undergoing 2,301,766 screening exams — 458,175 DBT and 1,843,591 2D digital mammography — were included in the retrospective study. The abnormal interpretation rate was 8.3% and cancer-detection rate was 5.8 per 1,000 exams.
With DBT, 97.6%, 91.8%, 75.0%, and 74.0% of assessed radiologists achieved the recommended acceptable performance ranges, respectively, for cancer-detection rate, sensitivity, abnormal interpretation rate and specificity.
The research was supported with funding from the National Cancer Institute (P01CA154292, R01CA262023, R50CA211115); the Patient-Centered Outcomes Research Institute Program Award (PCS-1504-30370), the National Cancer Institute (U54CA163303), and the Agency for Healthcare Research and Quality (R01 HS018366-01A1). Collection of Vermont Breast Cancer Surveillance System data was supported by the University of Vermont Cancer Center with funds generously awarded by the Lake Champlain Cancer Research Organization (032800).
The authors’ conflict-of-interest statements are in the published paper, which will be provided to journalists upon request.
Written by Linda Brooks at the Radiological Society of North America
For details about UW Medicine, please see our About page.
Topics:breast cancermammography