
In historic procedure, donor liver protects heart transplant
A UW Medicine team saved a patient with a dual-organ transplant based on a concept about immunoprotection.Media Contact: Brian Donohue - 206-543-7856, bdonohue@uw.edu

Doctors in Seattle are reporting a history-making case in which a patient received two donor organs, a liver and a heart, to prevent the extremely high likelihood that her body would reject a donor heart transplanted alone. In doing so, they successfully tested the concept that a donor liver can confer robust immunoprotection on a subsequent heart transplant.
The dual-organ recipient, Adriana Rodriguez, 31, of Bellingham, Washington, has recovered well since the Jan. 14, 2023, procedures, said Dr. Shin Lin, a cardiologist at the UW Medicine Heart Institute. He is the lead author of the paper describing the novel approach, newly published in The Journal of Heart and Lung Transplantation.

Heart-liver transplants to one recipient are seldom performed, Lin said. In fact, this was the first such case for UW Medicine surgeons. In cases previously reported in literature, the patients have needed the two grafts to replace both failing organs.
Rodriguez’s case was unprecedented in two ways: She received a donor liver only to mitigate the near-certainty, in her medical team’s opinion, that her body would immediately reject the donor heart she desperately needed. And her own healthy liver was transplanted, domino-like, into a second patient who had advanced liver disease.
“She met all criteria for transplant, but her antibodies (to the antigens of organ donors) were the highest we’ve ever seen,” Lin said. “Finding an immunologic match for her heart alone was going to be like trying to win the lottery. Essentially she would have needed the donor to be her immunologic twin.”
Rodriguez’s need for a heart transplant stemmed from a spontaneous tear within her coronary artery that occurred Dec. 7, 2022. Such “dissections,” in medical parlance, are rare but not unheard-of among women around the time of pregnancy.
Two weeks earlier, Rodriguez had given birth to her third child at PeaceHealth St. Joseph Medical Center in Bellingham.
“There are thought to be hormonal changes and stress in pregnancy that can make the coronary arteries vulnerable to these tears,” said Dr. Daniel Fishbein, a heart failure specialist on Rodriguez’s team. “In the best-case scenario, a dissection heals without much heart damage and the patient goes home with medications and gets better. But this patient had terrible heart failure.”

Rodriguez’s doctors at PeaceHealth initially treated the coronary artery dissection with an aortic balloon pump to help her heart circulate blood. Then they transferred her to UW Medicine, where doctors found that her dissection had caused widespread, permanent damage to her heart.
In the month that followed, Rodriguez’s team removed the balloon pump and employed other devices to try to supplant her heart’s pumping function.
“The dissection injured her heart a lot. We attempted to remove her from support over time to see if her heart was recovering, and she continued to fail that,” said Dr. Jay Pal, a cardiothoracic surgeon. “We went through a variety of support strategies to try to help her heal without ECMO and without transplant, but ultimately there was no other choice.”
On Dec. 14, doctors connected Rodriguez to an extracorporeal membrane oxygenation system (ECMO). This machine pumps and oxygenates blood, temporarily unburdening the patient’s heart and lungs. ECMO enables some patients to recover strength and forgo additional procedures, but in this case, Pal said, “going on ECMO meant she probably was going to need a transplant to get off ECMO.”
Rodriguez was officially listed for heart transplant on Jan. 5.
With every transplant, doctors measure the prospective recipient’s antibodies to gauge the likelihood of donor organ rejection. Someone whose levels are high is described as being “highly sensitized.”
“Pregnant women are more likely to have high sensitization because when they carry a child, their body develops antibodies against antigens that come from the father,” said Lin. “These antibodies don't attack the fetus, but if you transplant that person, those antibodies will attack the transplanted organ — sometimes within minutes.”
Rodriguez’s workup suggested she had a high likelihood of rejecting an organ from 99% of potential donors. Poring through medical literature for other ideas, Lin found an observational study from 2021 that noted a “profound immunologic protection” seen with a heart-after-liver transplant (HALT) protocol among seven highly sensitized patients who needed both organs.
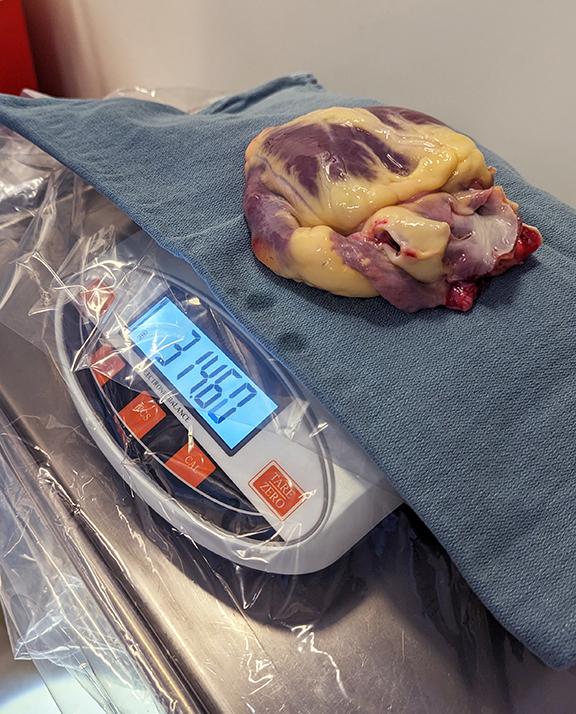
Although the data pool was too small to instill full confidence, and even though Rodriguez didn’t need a liver, Lin thought the HALT protocol was her best chance to survive. He proposed the idea to the team, with one amendment: Rodriguez’s healthy liver would be transplanted in parallel to another patient who needed that organ. HALT could become HALT-D, for domino.
Several of Lin’s colleagues initially were resistant.
“There was concern that this was an unproven treatment in a complex patient. But there were no other ideas or techniques that would allow this young mother to be free from ECMO and leave the hospital,” Pal said. “Dr. Lin’s unyielding belief that HALT-D would be successful convinced us. Ultimately, Adriana is alive and doing well because of his conviction."
On Jan. 14, organ-procurement agency LifeCenter Northwest notified UW Medicine that two organs had become available from a deceased donor. This set in motion a carefully orchestrated, 17-hour sequence at UW Medical Center-Montlake.
First, Drs. Mark Sturdevant and Ramasamy Bakthavatsalam removed Rodriguez’s liver and placed it on ice, then transplanted her with the donor liver. Drs. Pal and Ionnis Dimarakis then transplanted the donor heart while Sturdevant and Bakthavatsalam transplanted Rodriguez’s liver into a patient in an adjacent operating room.
“We looked at (Rodriguez’s) antibodies almost every day,” Lin recalled. “It was not until 65 days after transplant that her antibodies against these donor organs disappeared altogether. That’s when I felt like I could finally breathe easier. That meant it was an unqualified success.”
Exactly why a donor liver would protect a donor heart is still a bit of medical mystery, Fishbein suggested.
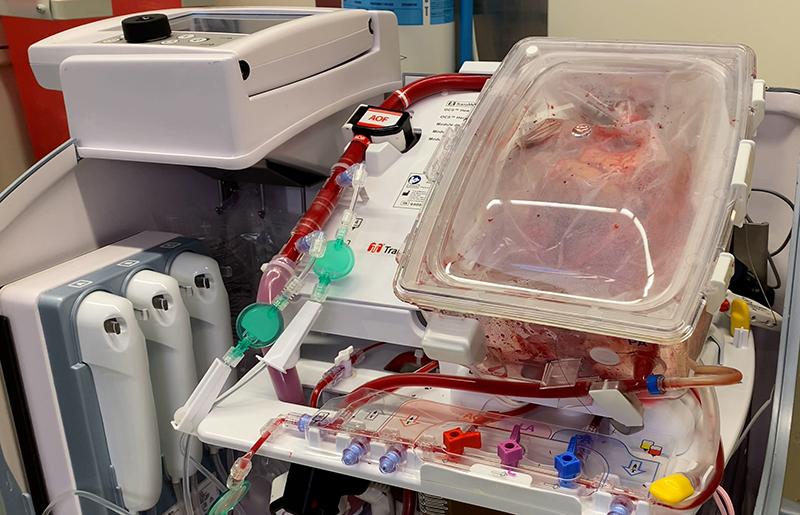
“I think we don't fully understand the science of transplant immunology. We can learn a lot from patients like this. We need to understand the magic so we can hopefully, someday, repeat it with medications instead of an organ.”
Six months out from her procedures, Adriana Rodriguez offered her thanks:
"There are no words to express my gratitude for my exceptional care — to the doctors and surgeons brainstorming on how to save my life, to my nurses for going the extra mile to make me feel comfortable, and to everyone working on my case who I didn't get to meet.
"I pray no other woman goes through this, but I hope my situation will benefit them and bring them hope," she said.
For details about UW Medicine, please visit https://uwmedicine.org/about.