
Common virus that besets transplant patients is study focus
UW Medicine will lead a $21 million national trial of a novel vaccine aimed to reduce the effects of cytomegalovirus in liver transplants.Media Contact: Brian Donohue - 206.543.7856, bdonohue@uw.edu
UW Medicine researchers will lead a $21 million, seven-year U.S. study of a novel vaccine’s ability to disarm a virus that causes graft failure and death in solid-organ transplant recipients.
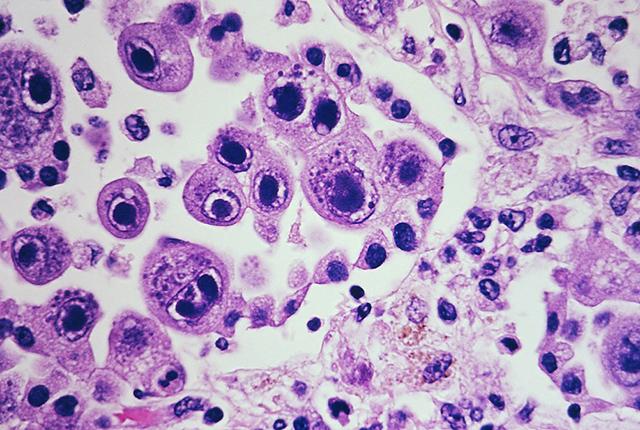
Cytomegalovirus, or CMV, is a common virus that most of us contract at some point, typically with little or no illness for people with healthy immune systems. But in immunocompromised transplant recipients, CMV can become a life-threatening infection.
“When a transplant recipient’s immune system is purposely stifled with medications to prevent rejection of the donor organ, their ability to fight off CMV is far less,” said Dr. Ajit Limaye. He directs the infectious-disease program for solid-organ transplant at UW Medicine.

Limaye and colleague Cynthia Fisher, both in the UW's Division of Allergy & Infectious Diseases, will co-lead a research project newly funded by the National Institute of Allergy and Infectious Diseases.
The clinical trial will involve 15 U.S. transplant programs and a vaccine candidate developed at the City of Hope cancer center in California. Researchers will study whether the vaccine, which has shown safety and efficacy in two small pilot trials, can keep CMV at bay in a larger population of liver-transplant recipients.
Cytomegalovirus can be transmitted in utero, via breast milk, blood and organ transplant, and the exchange of bodily secretions. As with other herpesviruses, CMV is a lifelong acquisition: Whether or not it causes illness, it remains latent in a body’s cells until death.
That makes transplant recipients vulnerable to CMV in two ways, Limaye explained.
“If the person has acquired the virus at some point before the transplant, latent CMV may reactivate as the patient’s immune system is tamped down to reduce organ rejection. If the person is sero-negative, meaning they’ve never had CMV, and they get an organ whose donor had CMV, there is a much higher risk for developing severe CMV infection because their body is getting hit with an unrecognized virus and their immune system’s ability to respond is way down.”
Given that about 8 in 10 adults have acquired CMV by age 70, the virus is familiar to transplant specialists. They employ antivirals to prevent or treat CMV when it emerges in organ recipients, but the drugs have toxic side effects and are costly. Moreover, CMV can develop resistance to them.
In the study, half of the patients will get the test vaccine pre-transplant and the other half will get a placebo. The investigators will study whether administering the vaccine enables patients’ immune systems to recognize CMV and to mount a sufficient defense.
Study collaborators at the City of Hope have developed a novel vaccine from modified vaccinia ankara. It includes genetic bits of CMV to provoke an immune response, but without replicating the virus.
“This vaccine aims not to generate antibodies but to muster T-cells and other immune-oriented cells to control CMV,” Limaye said. In preliminary tests, the vaccine was found safe in healthy volunteers and in a subsequent small study of stem-cell transplant recipients.
Although CMV’s specter shadows all transplants, this clinical trial involves only liver recipients, whose donor grafts and overall outcomes are most adversely affected by the virus, Limaye said. As well, the antiviral typically used against CMV in transplant, valcyte, is not approved by the Food and Drug Administration for use in liver cases, appearing to have more benefit for heart, kidney and pancreas recipients.
“Will those who were vaccinated tolerate the vaccine without significant side effects? Will they need less of the toxic antiviral drugs? Will they have less CMV infection than the people who got placebos? These will be primary measures of success,” Limaye said.
He projected that the trial would start recruiting liver-transplant candidates sometime in 2022.
The photo of "cytomegalovirus infection" was taken by Yale Rosen from USA, reprinted under CC BY-SA 2.0 via Wikimedia Commons.
For details about UW Medicine, please see our About page.