
Brain cells identified that may be key to unexplained pain
Activity of a cluster of neurons is necessary and sufficient to cause a common type of unexplained chronic pain called nociplastic pain.Media Contact: Leila Gray, leilag@uw.edu
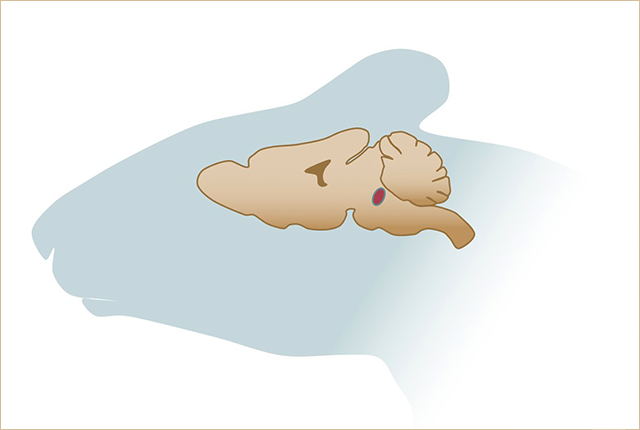
Stimulating a small cluster of neurons in the brain appears to create a response in mice that mimics nociplastic pain, a type of unexplained chronic pain that can affect people, researchers at the University of Washington School of Medicine in Seattle have found.
“When we stimulate these neurons, the mouse behaves as though gentle touch is very painful, which is one of the characteristics of nociplastic pain,” said Richard Palmiter, a professor of biochemistry and investigator of the Howard Hughes Medical Institute. Dr. Logan Condon, who spearheaded this research as a student in the UW School of Medicine's M.D./Ph.D. program, was lead author on the paper, which was published in Cell Reports.
The Centers for Disease Control and Prevention noted that during 2021 about 1 in 5 U.S. adults suffered from some form of chronic pain. The CDC declared that addressing chronic pain was a public health imperative because of its debilitating effects and potential consequences, such as depression and substance misuse.
Chronic pain can arise from ongoing injury or persistent damage to the nervous system. Pain caused by injury is called nociceptive from the Latin nocere “to harm.” Pain due to nerve damage is called neuropathic. But these categories do not explain a common form of chronic pain the persists even after an injury has fully healed and there is no evidence of neurological damage. This led the International Association for the Study of Pain to define a new category called nociplastic pain, meaning “able to be molded.”
Although the cause of nociplastic is unknown, scientists think it involves changes in pain circuits in the spinal cord and brain. These changes result in the perception of pain even when no nerve injury exists.
In the new study, researchers demonstrated that stimulating a cluster of cells in the brain’s parabrachial nucleus can generate chronic pain behavior typical of nociplastic pain. They also showed that inhibiting these cells can prevent pain from nerve injury.
The parabrachial nucleus is in an area of the brain known as the pons. It acts as a hub that relays aversive sensory information from the body to different parts of the brain. The parabrachial neurons found to create nociplastic pain are called Calca neurons, named for a defining gene for these cells.
“You can think of these Calca neurons as a warning system for the brain,” said Palmiter. “They respond to any aversive event you can think of — a pinch, a visual threat, a bad odor, a loud noise — and they tell your brain that something bad is happening in the environment and you’d better do something about it.”
It is possible to manipulate genetically defined neurons using viral techniques to express molecules that allow one to activate, or inhibit, those neurons.
The researchers also found that the nociplastic pain behavior continues even after the Calca-neuron activation has stopped. This suggests signals from the stimulated Calca neurons cause persistent effects — a sign of plasticity — in the nerve circuits leading to the spinal cord.
They also showed that it was possible to create nociplastic behaviors in the mice by exposing them to unpleasant, aversive experiences like nausea, chemotherapy drugs or migraine-like conditions.
Palmiter’s team is currently focusing on the neural circuits and plasticity that arises when parabrachial Calca neurons are activated.
“The brain is somehow sending signals to the spinal cord,” he said. “We want to figure out the pathway for those signals.”
This work was supported by grants from the National Institute on Drug Abuse (1F30DA057845-01) and the National Institute of Neurological Disease and Stroke (K00NS124190).
Written by Michael McCarthy
For details about UW Medicine, please visit https://uwmedicine.org/about.