
Study focus: kidney docs whose ill patients decline dialysis
How do clinicians respond to the sizable volume of patients with end-stage renal disease but who don't want conventional care?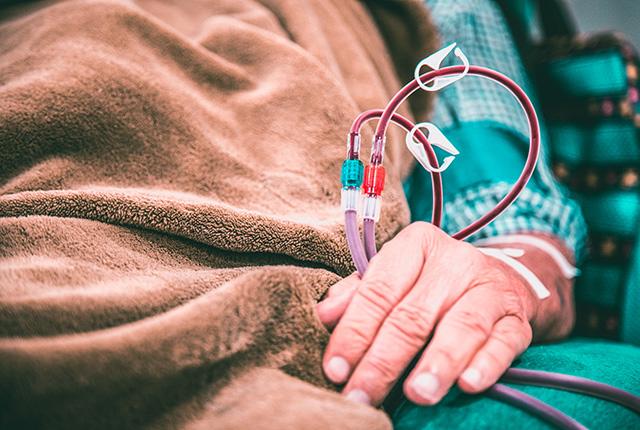
When medications and lifestyle accommodations stop helping someone fight advanced kidney disease, the person’s path forward narrows appreciably. Kidney doctors typically prescribe dialysis treatment, which, with luck, will extend the patient’s life until they qualify for an organ transplant.
There exists another path, though, in which the patient recognizes the paucity of available donor organs, the hardship of dialysis and its potentially limited benefit, and their current poor health—and makes a deliberate decision to decline the treatment.
What then?

“We don’t have a systemized way to track patients who choose against dialysis, so we have no way of evaluating whether we do a good job taking care of these patients after they make that choice,” said Dr. Susan Wong, a UW Medicine nephrologist who sees patients at the VA Puget Sound Health Care System.
She is leading a study that asks kidney specialists across the United States about their experiences caring for patients who are seeking a different path, and whether palliative care is offered instead of dialysis. She hopes to report findings in the fall.
Wong grew curious in recent years about patients who made this choice, as she was initially unclear how to support them.
“I couldn't answer basic questions like how much time do they have. What kind of resources are they eligible for? What kind of experience should they prepare for? I had tons of formal training on how to transition people to dialysis, tons on transplant, but I had not encountered somebody who didn't want to do dialysis unless they were in the ICU and facing multi-organ failure.”
In the United States about 600,000 people currently undergo dialysis and about 110,000 more are diagnosed ever year with end-stage renal disease (ESRD) — a number rising steadily.
In past research, Wong found that for about 1 in 7 VA patients eligible for dialysis, a decision is made not to pursue it. This suggests that the general population of ESRD patients with that conservative mindset is sizable.
Wong launched her survey of clinicians through the National Kidney Foundation and has heard back from more than 160 providers so far. She hopes the anecdotal findings will shed light on the extent to which conservative care is offered alongside dialysis and might hint at different ranges of care offered by practitioners across care settings.
The bigger-picture aim is to get nephrology specialists to recognize that a significant population of ESRD patients wants to face their last years untethered to a machine.
“Some doctors are uncomfortable broaching this idea because they feel duty-bound to try to save and extend patients’ lives,” Wong said. “Nephrologists should know that it’s important to lean into these conversations with patients, and that some patients want to know that choosing conservative care instead of dialysis is perfectly appropriate.”
Clinicians who discuss care options with ESRD patients are invited to respond to Wong's survey.
For details about UW Medicine, please see our About page.