
Dual-purpose scanner will shave minutes, save lives
Harborview and Fred Hutch radiologists welcome machines that they say will speed patient interventions and reduce complications.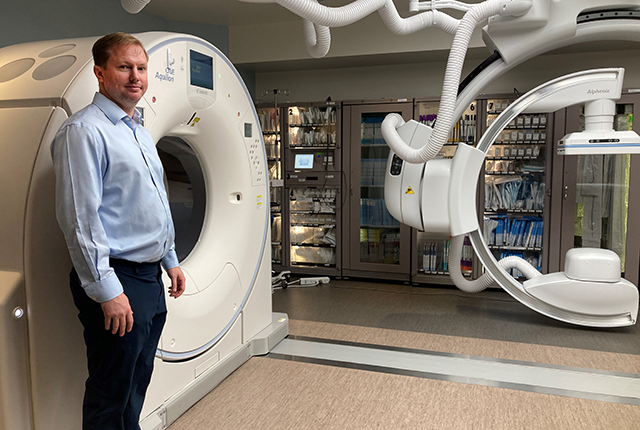
The Pacific Northwest’s busiest trauma-care site, Harborview Medical Center, last week formally welcomed its newest machine — one of only two such models in Washington state. It is expected to save lives and enhance patients’ recoveries.
The instrument combines 2D real-time, two-dimensional images (fluoroscopy) with high-res, 3D scans (computed tomography, or CT). Dr. Hugh McGregor, UW Medicine’s section chief of interventional radiology, explained its utility.
“Say someone was in a car accident and is in our trauma bay with serious injuries. Unless they go right to the OR (operating room), the first step is to get a CT scan to find out what is injured: Is it the spleen, the kidneys, the liver, the pelvis or all of those? Once that CT is read, the patient is triaged and may be referred to interventional radiology, which entails getting wheeled to another room where we will perform an angiogram and embolization (via fluoroscopy) to stop the bleeding.

“What this machine enables us to do is scan the patient in this room, get real-time high-res images to identify the bleeding, and then immediately start the embolization. It drastically cuts the time from diagnosis to intervention. And sometimes a few minutes can mean everything,” McGregor said.
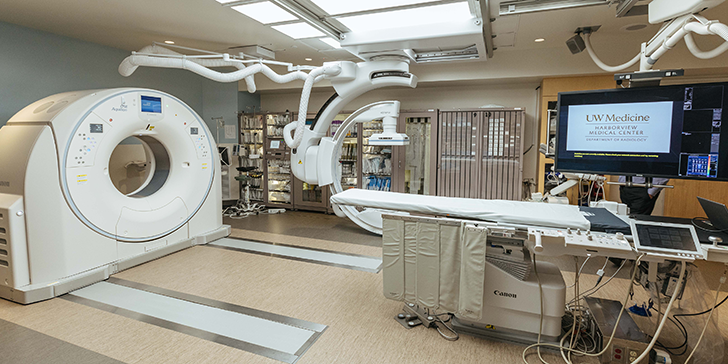
The machine, with a doughnut-shaped CT scanner and C-shaped arm for fluoroscopy-angiography, is manufactured by Canon Medical Systems USA. Only about 30 of these systems are currently deployed across the United States, said Yuji Hamada, the company’s president and CEO. He was the company’s lead representative in Seattle last week for ribbon-cutting ceremonies at Harborview and at the Fred Hutch Cancer Center, home to the other such machine in Washington.
Interventional radiologists like McGregor use these instruments to map vital organs, blood vessels and other structures, and then use those maps to guide thin wire catheters in minimally invasive procedures — for instance, to ablate tumors or remove blood clots or drain fluid from where it shouldn't be, like in the lungs.
“Typically we’ll treat the patient and keep them in the hospital for hours to days to watch for symptoms of complications. They go home, then come back in a few weeks for imaging to confirm that healing has happened as anticipated,” said Dr. Ethan Hua, who directs interventional radiology at Harborview. “This machine will help us better assess complications before the patient even leaves the hospital. We can do a CT immediately after a procedure to confirm and troubleshoot any complications.”
In cases where open surgery was once the norm, doctors increasingly perform catheter-based interventions like these for inpatients and outpatients, and in urgent and elective circumstances.
“Reliance on image-guided therapies is going up,” Hua said. “We’re looking for opportunities to intervene without surgery.”
For details about UW Medicine, please see our About page.