
Patients fare better with severe flu than with COVID-19
A study compared clinical features, lab results, and health outcomes of patients with the two conditions.Media Contact: Barbara Clements - bac60@uw.edu, 253.740.5043
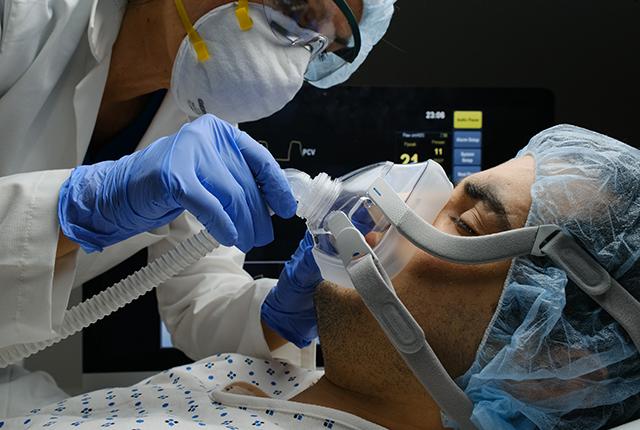
A study published today in the Annals of the American Thoracic Society reveals how patients hospitalized with severe COVID-19 fared, compared with those hospitalized with severe seasonal influenza. The study is believed to be the first in the United States to directly compare clinical features, laboratory results and health outcomes between patients with the two conditions.
Dr. Natalie L. Cobb, a UW Medicine physician in pulmonary, critical care and sleep medicine, and her co-authors reviewed the medical records of 65 patients critically ill with COVID-19 and 74 with severe influenza A or B who were admitted to the intensive care units of two UW Medicine hospitals between January 1, 2019, and April 15, 2020. This research was conducted as a retrospective cohort study—one that follows former patients who had common characteristics.
One key finding of the study was that the COVID-19 patients had an in-hospital death rate of 40%, versus 19% for influenza patients. This higher mortality rate was independent of the patients’ age, gender, co-occurring health conditions, and severity of illness while in the ICU.
Patients with either condition frequently required mechanical ventilation. Compared with those with influenza, however, patients with COVID-19 needed to remain on mechanical ventilation longer and had worse lung functioning overall. Patients with COVID-19 were also more likely to develop acute respiratory distress syndrome, or ARDS, a life-threatening complication in which the lungs become severely inflamed.
“The finding that ARDS may be more prevalent among critically ill patients with COVID is important in understanding why there may be a mortality difference between the two diseases,” Cobb said. “We also found that patients with ARDS due to COVID-19 had a trend toward worse clinical outcomes than ARDS patients with influenza.”
The researchers looked at characteristics of patients in the two groups. COVID-19 patients had slower improvements in blood-oxygen levels, longer durations of mechanical ventilation, and lower rates of extubation (removal of breathing tubes) than the influenza patients. Patients with COVID-19 were also more likely to be male, have higher body mass index and higher rates of chronic kidney disease and diabetes.
Nearly four times as many COVID-19 patients identified as Hispanic as did influenza patients. The authors suggest that this difference may be related to underlying health factors as well as to social and economic inequalities.
The researchers noted that, early in the COVID outbreak, many comparisons were made between COVID-19 and infection with influenza, which is responsible for a significant number of hospitalizations and deaths, both in the United States and globally. While previous studies did not directly compare the two diseases, research has shown that important differences exist between the two diseases in the proportion of individuals with severe illness and mortality.
As the flu season continue, it is likely that the nation is experiencing another surge in COVID-19 cases, Cobb said she thinks the findings present real-world public health implications.
“With rising cases of COVID-19 and the flu season, which began in October, it is possible that we may see spikes in hospitalizations and ICU admissions that could overwhelm our healthcare system,” she said. “I strongly encourage people to get the flu vaccine and continue social distancing measures and masking to limit the spread of COVID-19.”
She added, “Our findings underscore the importance of efforts for limiting transmission as well as ongoing investigations for effective therapies and vaccines.”
For details about UW Medicine, please see our About page.